During his talk at the 2018 Skin of Color Seminar Series (now known as the Skin of Color Update), Dr. Seemal Desai discussed the treatment of melasma (post inflammatory hyperpigmentation PIH) with a particular emphasis on new and emerging therapies. Dr. Bridget Kaufman, onsite correspondent for the meeting, shares highlights directly from the talk. *Clinical pearls* from this session are bolded, underlined, and marked with asterisks.
Dr. Desai started by stressing the importance of having an honest and upfront conversation with your melasma patients about realistic expectations for treatment. *You must emphasize to patients that this is a chronic condition and set their expectations accordingly.*While improvement with treatment is likely, there will always be underlying pigmentary changes even despite treatment. Patients must understand from the beginning that they cannot be cured of this condition.
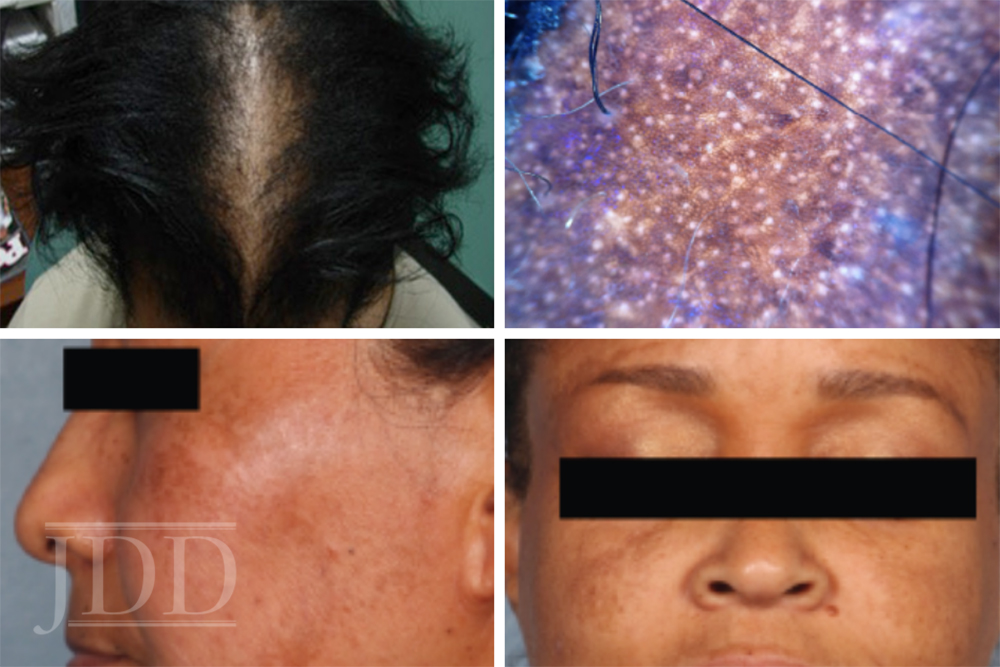
Dr. Desai then addressed the large vasodilatation/vascular component of melasma. Although the predominant feature of melasma is the hyperpigmented patch, a pink hue becomes apparent after treatment of the brown pigment. Historically, the redness was thought to be a side effect of Modified Kligman’s Formula, but more recent research suggests that this due to an inherent expression of vascular markers in melasma lesions. This vascular component can be treated with low fluence pulsed dye laser; oral tranexamic acid has also been helpful in Dr. Desai’s practice.
Dr. Desai then addressed the relationship between thyroid disease and melasma. There are a few studies showing thyroid disease in patients with recalcitrant melasma. *If, after optimal treatment, a patient does not improve within 3-6 months, you may want to get a free T4 and TSH to screen for thyroid disease.*
So now onto the treatment of melasma! Given that triple combination cream (TCC) is the gold standard therapy for melasma, it makes sense that Dr. Desai started with a discussion of research on this product. A randomized controlled trial of TCC in Southeast and East Asian patients with melasma found that, after 8 weeks of treatment, *TCC was superior to monotherapy with hydroquinone, although it was associated with more adverse effects.* Dr. Desai has found this to be true in his practice and, therefore, he rarely prescribes hydroquinone alone. The retinoid and steroid in TCC help with desquamation and exhibit anti-inflammatory properties that counter the upregulation of prostaglandins and tyrosinase in melasma.
For more pearls like this – register for Skin of Color Update in NYC now before it is sold out.
Read more.
Excerpt provided with permission. Originally published by Next Steps in Dermatology. All rights reserved.